On July 10, 2016, I set out with one of my best friends to run the Maroon Bells Four Pass Loop, a 27-mile trail with 8,000 feet of elevation gain that hits four 12,500-foot mountain passes in the Maroon Bells Wilderness Area near Aspen, Colorado. After a summer of running America, I was excited to return west and tackle another run on my ultra-running bucket list. The run was destined to be great.
But this run turned into the scariest experience of my life. By midnight that same day--17 hours after we'd left the trailhead at 5 a.m., and several hours past the absolute latest we anticipated being on the trails--I was passed out, convulsing and vomiting violently, stuck at 11,000 feet above sea level in the Rocky Mountain wilderness. I would later learn that I had high altitude cerebral edema (HACE), high altitude pulmonary edema (HAPE), and hyponatremia--and I was on the brink of death.
Thanks to the heroic efforts of my friend, a trio of backpackers, Mountain Rescue Aspen search and rescue team members, Pitkin County Sheriff's Office deputies, and a Flight for Life Colorado helicopter flight team, I made it out alive.
Today, exactly one year later, I have made a 100% recovery on all fronts. My brain is back to normal, my body is back to normal, my spirit is back to normal--I am me again. Not only that, I ran my first 100-mile race(!). I feel lucky and thankful in more ways than I can express. I wanted to share my story, in the hope that it sheds light on the risks that go with adventuring at high altitudes--and how disaster can strike when you least expect it.
http://www.alltrails.com/events/2014/07/aspen-4-pass-loop-backpack
A PLAN
Everything starts with a dream. Each of us has something we aspire towards, whether it be a promotion at work, an achievement in one's family life, or something else. For me, a lot of my little dreams revolve around running. (I've already explained all of the reasons why I run here.) So when my good friend, Will, proposed a trip out to the Aspen/Snowmass area of Colorado, my first instinct was to identify a dream trail run in a dream running area of the country. I was especially aware that my "Wookie Runs America" running road trip of the previous summer had skipped Colorado entirely. There was no excuse now: if we were going to Aspen, we had to run in the mountains.
With that dream conjured up, plans were set in motion to run the Maroon Bells Four Pass Loop. It had all the elements of the perfect ultra-run: challenging, epic, beautiful, fun, wild.
http://www.hikingwalking.com/destinations/co/co_cent/aspen/four_pass_loop
Not lost on me was that the Four Pass Loop was also popular. Sure, it was in a wilderness area, but we were bound to see plenty of hikers and backpackers along the way. After a summer of running alone (always with a personal locator beacon), I had become attuned to finding runs on which I was more likely to bump into people. Never did I want to be completely alone. There was always safety--or at least comfort--in numbers. This run was no different.
ARRIVAL
I left my home in D.C. at the crack of dawn on Friday, July 8, giddy about the trip ahead. I flew directly into Aspen-Pitkin County Airport, eager to save time by skipping the 3-hour drive from Denver through the Front Range. That was probably my first mistake. For a sea level-living person like me, Aspen, at 7,900 feet above sea level, is at relatively high altitude. And our hotel, which was actually in Snowmass, was even higher, at 8,200 feet. No matter how fit I was as a runner, vaulting straight up to that elevation so quickly had some non-zero chance of messing with my system. Probably a better choice would have been to fly into Denver, at 5,200 feet, and maybe even spend a day acclimating there. (Will had done exactly this, flying into Denver 2-3 days earlier, and exploring the city's breweries until I arrived.)
Still, I felt okay with my decision. I'd spent a chunk of time reading about altitude sickness--how to avoid it, as well as how to recognize and address it if it arose. To that end, I told Will that we should do essentially nothing on Friday to let our bodies adjust. So all we did was catch up over a couple beers, do some work on our laptops, and take a stroll through downtown Aspen.
Catching up over beers and catching up on work.
Downtown Aspen.
By about 5 pm, as we made our way to our lodging in Snowmass, I felt the first signs of a headache. It was mild, but it was there. I thought it might be the beer. But I'd only had two, and I'd been following up with plenty of water. My urine was straw colored--exactly what I wanted it to be. So I figured it must be something else. It must be the altitude.
I began closely monitoring how I was feeling because our original plan was to run the Maroon Bells beginning at 5 a.m. the next morning--i.e., Saturday, July 9. But by 7 p.m., after a quick dip in the lodge's pool, and over dinner, it had become obvious that that would be a poor decision. I could still feel a headache. It wasn't painful, but it just didn't feel normal. I told Will that I didn't want to take any chances. I needed more time to acclimate. Would it be okay if we pushed back our run to Sunday?
Taking a dip.
Will, being the reasonable guy that he is, agreed with my decision. He may have poked fun at me just a tad, but he knew that I knew my body best, and that altitude was the one variable that we had agreed we could not mess with. All the previous times I'd spent at high altitude--elevations between 10,000 and 13,000 feet--I'd never had any altitude issues, not even the slightest of headaches. And I was not about to let this first time mess me up any more than I felt it already was. We ended up going to bed early, at 8:30 p.m. Again, if the goal was to get acclimated, rest and relaxation was key.
ACCLIMATION
Saturday morning, I woke up at around 6:30 a.m., feeling extremely well-rested and ready to take on the day. This was the best sleep I'd gotten in weeks. I immediately noticed the headache was gone, so I decided I'd test out my mountain legs and lungs by going on a short, easy run up the ski slope at Snowmass. I spent about 30 minutes going just over 3 miles, keeping my heart rate low and not even pushing up or down the 700 feet of vertical that I chose to tackle. I was barely sweating, and I felt really, really good. My legs, body, and mind were all in check. I knew at that point that I'd be ready for the Four Pass Loop the following morning.
Running up Snowmass.
After returning to the lodge, Will and I geared up to go downhill mountain biking. This was something that Will had really wanted to do. I wasn't as dead set on this part of the trip, but I was also curious about the whole experience, as I'd also never done it before. At 9 a.m., we suited up and began going up-mountain in the gondola, and cruising downhill on our downhill mountain bikes. It was thrilling.
Downhill mountain biking pads--AKA the Mad Max life.
Despite all the pads involved, downhill mountain biking is not very strenuous. You practically don't pedal and instead use your momentum to take you down the mountain. The shocks on the bike are really deep, which makes for a relatively smooth ride. The parts of the body that hurt the most after a day of downhill mountain biking were our hands, which had rattled over the various roots and rocks on the trails. One thing that I probably should have accounted for was the altitude. We'd taken the Elk Camp gondola up 6 times to 11,325 feet. It is hard to say if this biking outing amplified any issues. I didn't feel any headaches all day, and we barely sweated while doing this. We also had our Camelbaks the entire day and were constantly hydrating. In retrospect, spending all that time above 11,000 feet did not help.
At 3 p.m., after a solid lunch break, we returned our bikes and pads and headed back to the lodge. We'd seen the New Belgium Ranger Station, and figured it would be fun to work there while carbing up for the following morning. So that's what we did. Over the course of 3 hours, I had one beer, several pretzels, and a hearty chicken dinner. I checked my head--no headaches! By 7 p.m., after a quick dip in the pool, we returned to our room and repacked our gear for the day ahead. We cut no corners. We each packed a dozen energy bars (one per hour for that many hours, even though we anticipated finishing within 10-12 hours). I had my water filter, topo maps, a trail guide, a compass, and gear for bad weather. I even had my emergency bivvy, just in case something went wrong and we got really, really cold. (I joked to Will that I would share the small space with him, if it came to it.) Will brought a med kit. By 9 p.m., we had our eyes shut, excited about the long day ahead.
My outfit for the day ahead. Obviously, it includes a November Project-tagged shirt.
ADVENTURE
Sunday, July 10. We rise at 4 a.m., despite Will's protests. I tell him that the more distance we cover early on, the better. Thunderstorms are unpredictable in the afternoon. Plus, I want to leave as much margin for error as possible. The goal is to be done with the run many hours before sunset--ideally by 3 p.m. So we plan to start running from the trailhead at 5 a.m. sharp. We are close. We get to the parking lot at the trailhead just before 5 a.m., but I need time to deal with a pre-run bowel movement (as always). We start at 5:15 a.m., only 15 minutes after our target time. The first views of the Maroon Bells in the pre-dawn cool are stunning.
5:29 a.m.
And just like that we are off! The trailhead is at 9,580 feet, which is higher than where we'd slept, but not as high as where we'd reached by gondola several times the day before. Our first segment has us going clockwise over West Maroon Pass, up to 12,500 feet. We begin making steady progress up towards the pass, passing a brunching moose, and many incredible morning sights along the way.
5:34 a.m. Spotting a moose.
5:47 a.m. Still within the forest.
6:01 a.m. Escaping the trees.
6:16 a.m. First light on the mountains.
6:17 a.m. Blending in with the wildflowers.
6:20 a.m. Running towards West Maroon Pass.
Everything feels really good at this point. Our legs are fresh, our minds are clear, we are eager to make progress, and the weather cannot be more ideal. It is just chilly enough that walking feels cold, but as long as we are jogging slowly, we are warm enough.
Our pace is relaxed. I had told Will in an earlier email that the idea was "slow jogging", that "our heart rates would be low", and that I expected to feel completely normal--maybe just a tad sore--the next day. This was not a race. (I wore my heart rate monitor the entire day and ensured we stayed completely aerobic. Unfortunately, I lost the heart rate data, which would have been interesting to analyze, because my watch ran out of battery.)
The serenity of running into the sunrise is one of the best things about trail running. The mountains around us wake up. Light begins to creep down from the tops of the mountains. We soak it all in.
7:53 a.m. The sun is coming up.
About 3 hours in, and we are making our first ascent towards West Maroon Pass. The plan on the ascents is to hike. There is no point in burning our legs by running. That risks leaving us out of gas--not something we want to do out here. We take lots of breaks for photos, which adds more rest. Also, Will cannot get enough of the wildflowers. I indulge his desires.
8:29 a.m. Will cannot get enough of the wildflowers.
3.5 hours in, and we make it up to our first of four passes. The blast of wind that hits us as we crest the pass is powerful. On one side, it is still and warm. On the other, it is windy and chilly. Life is good.
8:50 a.m. Panoramic view from West Maroon Pass--stunning colors.
We look where we came from.
8:53 a.m. Where we came from.
And we look where we are going.
8:53 a.m. Where we are headed.
I am still feeling very strong. Not fatigued in the least, not dehydrated in the least, well-fed, and just super happy with how our day is going. The picture probably shows it here, but there are no real signs for concern right now. We are both all smiles.
8:56 a.m. Pass #1 complete!
From West Maroon Pass, we drop about 1,000 feet into Purity Basin and skirt our way northwest under the ridge-line towards Frigid Air Pass. By 10 a.m., we are making the relatively short ascent--the shortest of the 4 for the day--up to Frigid Air Pass. Will recalls that it was during this ascent, nearly 5 hours after we'd started our run, that I hold my head for the first time. Apparently, I deny that I have a headache. I was still fully conscious. I may have held my head, but I certainly do not feel any pain or other cause for concern.
10:08 a.m. Pass #2--Frigid Air Pass!
The descent from Frigid Air Pass into Fravert Basin is swift and steep. The rocks are slippery, and there is little room for error. These challenging and dangerous ascents later become extremely treacherous once my condition begins devolving. Right now, they are easy, as I'd spent the entirety of last summer tackling terrain just like, or harder, than this.
10:11 a.m. Descending the back side of Frigid Air Pass.
Once we are down in the Basin, we make steady progress again towards the North Fork and Trail Rider Pass, which would be our penultimate pass. We are probably 12 miles in at this point. A bit shy of the halfway mark in just over 5 hours. We are off track to finish in 10 hours, but it seems we will finish within 12 hours--exactly within the time scale I had projected.
10:27 a.m. Heading towards Fravert Basin and the base of the 3rd pass.
At around 11 a.m., things slowly begin to go wrong. The first thing I notice is that, as we are traversing Fravert Basin, my running pace has slowed down relative to Will's. Up until this point, we'd been running a steady, consistent pace--together. I don't necessarily feel more tired. I check my heart rate and it's still safely in the aerobic zone. Yet, as we cross the Basin, something just feels off, and I begin dropping behind Will as he cruises ahead. At 11:06 a.m., Will notices that I stumble over several places on the trail with unchallenging footing. When Will asks how I am doing, I tell him I have a headache. I tell him I'll monitor the situation. Internally, I begin thinking, "do we turn around?"
At 11:11 a.m., I take a photo of Will with the mountains near Maroon Peak in the background. It is the last photo I will take that day.
11:11 a.m. The last photo I took that day.
ABORT MISSION
We descend further into the Basin, and begin approaching the base of the climb to the third pass. My head begins hurting more, so we decide to stop, take a water break, take some ibuprofen from the med kit, and then decide on a course of action. As we sit on the side of the trail, I feel hazy. This is not normal. I tell Will we have to abort the run.
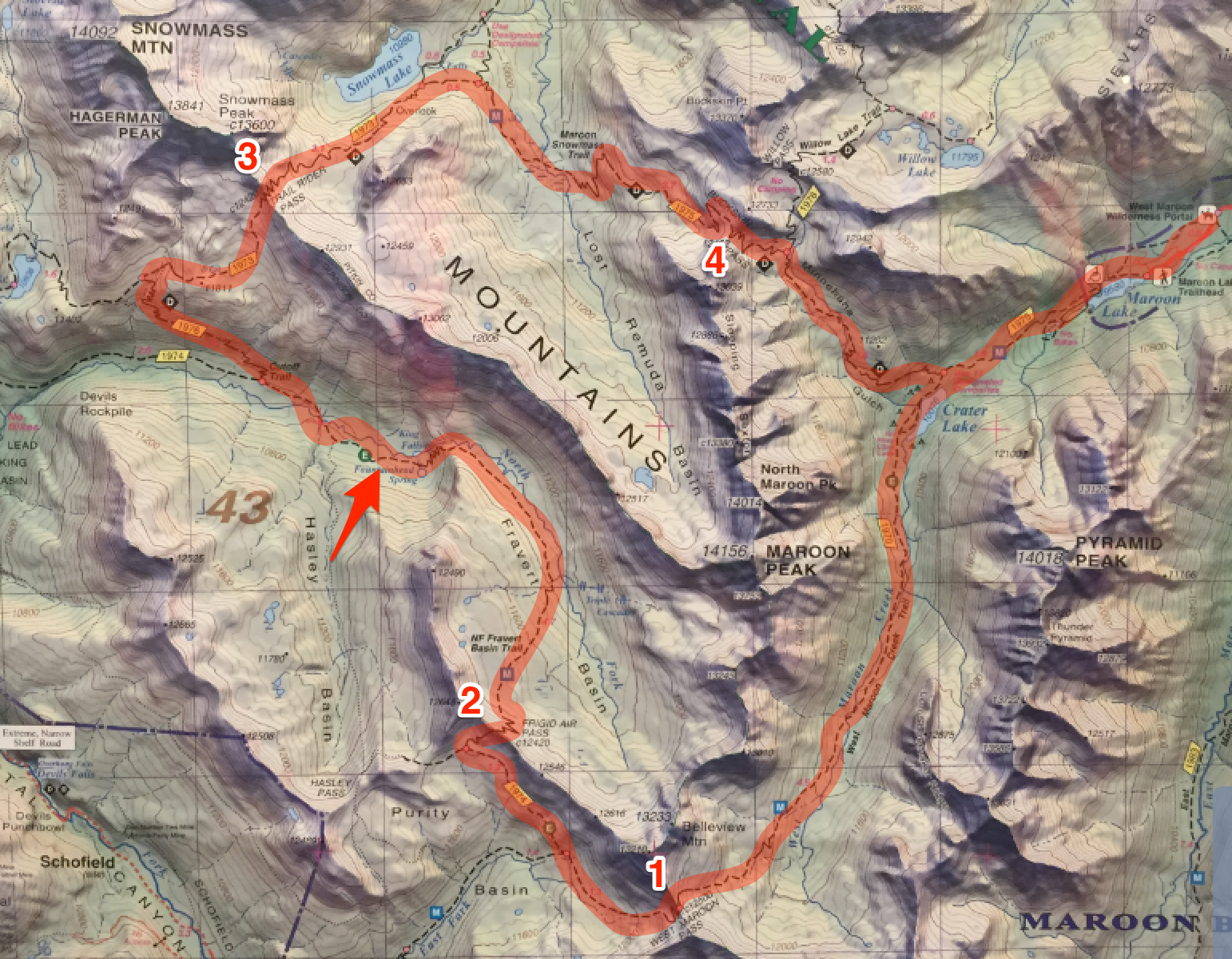
We could not have been in a worse location to decide to call it quits. We were almost smack dab at the bottom of the valley between the 2nd and 3rd passes--just about the most remote place we could be on the Four Pass Loop:
After taking stock of our situation, we see two clear options, and one not-so-clear one.
Option one is to continue forward and finish the loop. At this point, we are about 13 or 14 miles in, so this option would require the shortest distance out to the trailhead. At the same time, I know from having studied the elevation profile in the days leading up to the run that the last two passes--Trail Rider and Buckskin--involve two serious ascents. They will be unrelenting, and will also put us even further into unknown territory. That could be risky.
Option two is to turn around and backtrack the way we came. This requires a couple more miles of distance, but it has the advantage of having only a mini-descent and mini-ascent between the second and first passes. Another bonus is that we are completely familiar with this route and will have the mental advantage of knowing the terrain as we make our way out.
Option three is less well-understood. Looking at the topo map that I had, I can see that if we continue forward but turn left at the next juncture (instead of right up to Trail Rider Pass), we can hit Silver Creek Trailhead. The plus side to this is that it seems shorter than the first two options, and will give us the chance to potentially hitchhike our way to a lower elevation at a faster rate. The big downside is that we know nothing about the conditions of this trail, or how well-trafficked the mining road is, or whether it even makes sense to head further away from a known quantity and deeper into the wilderness.
My judgment is a bit cloudy at this point, as my headache is intensifying, but we are strongly leaning towards option two. We do not want to take the risk of the two major climbs ahead of us. We do not want to take the risk of going off the main loop and heading towards an unknown trail and destination. If we turn around, everything would be a known quantity, and that would also make breaking down the day into chunks mentally much easier.
Almost as if someone hears our plight, two rangers appear out of nowhere. They are heading towards us from the opposite direction. They stop and ask how we were doing. I explain my situation, and they advise us to turn around. (They also confirm that option three is better than option one because the tiny mining town of Marble is at the bottom of the mining road that leads to the trailhead, but that it is still a much worse idea than option two.) We had made the right decision originally, but it is nice to get confirmation from experts in the field.
FADE TO BLACK
It is 11:30 a.m. when we finally turn around and begin heading back up the Basin towards Frigid Air Pass. At this point, I still have my wits about me, and I realize the situation we're in. I am weak, lightheaded, approaching delirium--and we have two passes and several thousand feet to climb. I never imagine that I won't make it back to the trailhead and to the safety of civilization on my own two feet. I know I will struggle, and I know I will hurt, and I know I will feel fear, but I also know I am going to make it out. How could I imagine anything else?
At the same time, I know getting out is no laughing matter. I set my mind to escaping the mountains safely, with Will's help. There is no more time to take photos. We need to move deliberately, because my condition is only getting worse. And the only cure for altitude sickness is to descend from elevation as rapidly as possible. This is now our primary goal because, again, we do not want this day to end in anything but happiness on our parts. (Plus, I have a job to get back to the next day in D.C.)
Beginning at noon, I begin struggling more. My memory of this period is spotty, but Will tells me that I am moving just as quickly as we had been moving before. When we pass the rangers again, they and Will both advise me to slow down. I don't know what has gotten into me, but I'm guessing I probably think that moving quickly up and out of the basin is the most prudent thing to do. I am probably scared that I won't make it out. But with a rapidly deteriorating brain and body, I need to move cautiously, in a way that will not overtax my taxed body. We need, in other words, to find the perfect balance. Around this time, Will offers to take my pack. I take him up on the offer and thank him because every load off my back will help me move quicker. I keep my trekking poles for balance, and we continue uphill.
Just before 2 p.m. and we are at the base of Frigid Air Pass, about to begin the ascent. I feel wretched. I express to Will that I am losing my vision. My biggest concern at this point is falling off a switchback on the ascent over the pass. With my normally decent balance, the ascent would have been no issue. But impaired and wobbly as I have become, I know that stumbling off a cliff is a distinct possibility. This scares me, and I express that to Will over and over again. As we amble up the pass, I fall several dozen times, thankfully mostly uphill, because I am leaning my head and crouching down in that direction. A couple times, I fall downhill, but Will is there to catch me by my armpits.
At 2:30 p.m., we reach Frigid Air Pass. We bump into three hikers. I ask them if they have any spare ibuprofen for my splitting headache. They do, and offer me 3 pills. I tell them about how shit had hit the fan in the last couple hours and I am barely able to put one foot in front of the other. For the first time, I realize how quickly things are spiraling out of control, and I panic. Then, in the presence of these innocent hikers, I break down for the first time. It is a controlled sob, and doesn't last much more than a minute. For the first time, I begin to think that I won't actually make it off the loop alive. I quickly compose myself. I have no energy to waste, especially not on tears. I am more determined than ever to make it out. We thank the hikers, say goodbye, and begin our descent towards West Maroon Pass, which will be our last vertical hurdle to overcome.
Our bump-in with those hikers, and my breakdown in front of them, are the last memories I have of our day on the Four Pass Loop.
RESCUE
I have no memory of what follows, which occurred after I blacked out. The below is based on the chronology that Will later created for the medical professionals who cared for me. It is also based on multiple conversations I later had with Mountain Rescue Aspen and the three backpackers--Erik, Robert, and Shane--who took care of me.
Will notices that my condition improves as we head down Frigid Air Pass and into the basin once more. As we begin the traverse towards the base of the final ascent, I begin moving more quickly.
At 3:30 p.m., we ascend West Maroon Pass--our last major obstacle. If I can get over this, it is literally all downhill from here. I am determined to make it--and am in complete survival mode--so nothing is stopping me. Will notices that I appear more mentally ready for the challenge of this final climb. At the same time, he notices that I struggle to the same degree as our wobbly ascent of Frigid Air Pass.
At 4:00 p.m., we have made it over West Maroon Pass. Miraculously, I have made it over--with Will's help. We are now optimistic that we are going to get off the trail and down-mountain in sufficient time. But as soon as we start descending, Will notices that I do not move nearly as easily or quickly as I did while descending Frigid Air Pass.
By 5 p.m., I cannot walk on my own. I stumble forward like a drunkard while Will follows closely behind me and catches me about every ten steps. This progresses to Will walking next to me with one hand on my neck and another in my armpit. I begin stopping and asking, "Where do we go?" I do this even when there is one clear and obvious direction.
By 6:30 p.m., I am aimlessly shuffling my feet forward while Will keeps his hands in my armpits, and I lean back. I begin spitting clear spit, and making noises that sound like a precursor to vomiting. I don't say I need to vomit though.
At 7 p.m., I become non-verbal.
At 7:20 p.m., we encounter three backpackers--Erik, Robert, and Shane--heading up the trail as we are coming down it. Will asks them if they can stay with me at the West Maroon Creek Crossing. They agree and help Will carry me to the Creek. According to Erik, at this time, I "looked really bad, and could barely stand." (Erik, Robert, and Shane created a video of the night of my rescue, from which I derived additional information.)
At 7:40 p.m., Will leaves our remaining food and water filter with me and the backpackers. Will crosses the creek and runs back to the parking lot, which is only a few miles away. As he runs, he has thoughts ranging from "I think he's going to die" to "maybe I'm completely overblowing it."
Meanwhile, back up in the Maroon Bells with the backpackers, I begin to vomit, and also experience seizures. Erik, who has EMT training, tries to keep me on my side, to prevent aspiration.
Robert, Erik, and Shane taking care of me.
At 8:10 p.m., Will arrives back at the parking lot and begins driving back towards Aspen looking for cell reception. By 8:30 p.m., he gains cell service, and calls the Aspen non-emergency number to request help. The operator says that a ranger will call Will back within an unspecified time-frame. Concerned by the lack of urgency, Will calls his parents, who are doctors, seeking their opinions. They insist that this is urgent and that Will needs to call 911. Will calls 911 and insists that I need immediate attention. The Sheriff's Department notifies Mountain Rescue Aspen. At 10 p.m., Will meets the deputy sheriff, who leads him to the Mountain Rescue Aspen Rescue Center. Will describes my symptoms and location to the rescue team.
At 10:15 p.m., according to Robert, I am "status quo--not getting any worse, not getting any better." I continue to vomit, throwing up bile.
By 10:50 p.m., Aspen Mountain Rescue deploys a team of four with oxygen to find me.
At 11:45 p.m., according to Robert, I am "about the same as [I] was before." He believes that the rescue operation won't begin until daybreak, so thinks "we're just going to have to ride it out." (Erik and Robert later recount their anxiety in thinking that no one was coming that night, and that I was going to die.)
Just after midnight, Mountain Rescue Aspen makes contact. According to Mountain Rescue Aspen I am unresponsive, and shaking uncontrollably. I am still breathing and have a pulse, but don't respond to the high-flow oxygen they immediately administer. The doctor in the team takes one look at me and instantly determines to request a medivac--a Flight For Life Colorado helicopter from St. Anthony Hospital in the town of Lakewood, just west of Denver.
Mountain Rescue Aspen--assisted by Erik, Robert, and Shane--work to prepare me for the medivac:



Shortly after 1:00 a.m., the helicopter arrives but can't find a place to land. The team works to clear a 100-foot-by-100-foot bed for the helicopter to land. Another 8 members of Mountain Rescue Aspen arrive. After several minutes of testing landing spots, the helicopter lands at the Maroon Creek Crossing and the team straps me in. By 1:30 a.m., the helicopter takes off for St. Anthony Hospital.
Flight for Life Colorado's Eurocopter AS 350 "AStar" B3 helicopter.
At 3 a.m., the helicopter arrives on the helipad at St. Anthony hospital, where I'm immediately taken into the ICU.
WAKING UP
I can barely recall it now, but the first memories I had after the incident were created as I was drifting in and out of consciousness. I remember feeling like I was drowning. I didn't know it then, but I had been intubated, and the tube that had gone down my airway was triggering a choking sensation. That sensation is what woke me from my coma (or at least that's how I remember it).
When I first gained consciousness, I felt voiceless and weak. Something was down my throat, and I wanted to get it out immediately. Blurry objects surrounded me, but I had no sense of place. When I finally recognized that these blobs were humans, I tried to yell "I'm choking!" to grab their attention. But I had no words. The tube prevented me from speaking. I felt like a soul trapped in a lifeless body. I began moving my arm to yank out whatever it was that was shoved down my throat, but my hands felt immediate resistance. They had been restrained (in what the nurses called "hand jail").
Somehow, I managed to grunt and harrumph and get the attention of a human. I tried my darnedest to sound out recognizable words. "I. Am. Choking." Nothing came out. Finally, someone asked me if I wanted to write out a message. I nodded my head. But as soon as I felt my hands being untied, I instinctively whipped up one hand towards my mouth, clutched the tube that I realized had been stuck down my throat, and yanked at it. And thus began a hospital room tussle. A flurry of bodies surrounded me, and once again put my arms in hand jail. My attempt at freedom had been stymied.
I drifted again into unconsciousness.
When I awoke again--this time for real--I remember hearing familiar voices. I opened my eyes and looked around. Why were my parents talking to me? Why were various friends--including several I hadn't seen in several years--crowded around me? Why was I in a hospital bed? None of it made sense.
But then, a spurt of memories came back. I remembered that I had set out with Will to run the Four Pass Loop. And then I also remembered: something had gone wrong. The details escaped me, but I knew that I was in the hospital because I had not "made it out" as Will and I had originally planned when we decided to turn around and retrace our steps.
Everything was foggy. I appeared to know things, but didn't really know them. And I realized that there were many things I didn't remember at all, at least initially. When someone confirmed that I had been in a coma for 3 days and that it was already Wednesday, I immediately asked for my laptop so that I could let my coworkers know what had happened (as if they hadn't already been informed!). Will passed me my computer, but I pushed it away. I insisted it wasn't mine because my laptop didn't have a brown case, like this one did. After arguing back and forth with Will, it finally dawned on me that I'd bought a new case a few weeks earlier. Sheepishly, I took the laptop back.
I flipped open the laptop and the login screen popped up. I put my hands on the keyboard, index fingers on the F and J keys (just as I'd been taught in elementary school)--and then I stared blankly at the screen. I had forgotten my password. I typed in several common passwords that I recalled using in the past. They didn't work. I also realized that my motor coordination was weak. I switched to typing with a single finger. I typed out several other passwords. These didn't work, either.
I can't remember how things finally clicked again, but my password eventually came back to me a few hours later. The mental energy needed to recall that one double-digit string of numbers and characters was extraordinary. I passed out again.
Trying (and failing) to log into my computer.
RECOVERY: COLORADO
The road to recovery was hard. And slow. And painful. It involved more doctors and nurses and health care professionals than I can remember (and here I want to show my unyielding love and thanks to each for taking care of me and getting me back on the right track--THANK YOU!). It involved countless tests--ranging from x-rays to CT scans to EEGs to EKGs to other things I cannot even name or even recall. All I have to memorialize this period of my life is the 3-inch stack of medical bills that meticulously catalog the drugs that went into my body, and the treatments my body received, during my hospital stay.
I have a few photos of this grim and painful period of my life. But this photo best encapsulates the mood I was in during my first week at St. Anthony:
That stay also involved rounds of occupational therapy, speech therapy, and physical therapy--all of which I undoubtedly needed. Bit by bit, these sessions brushed off the cognitive cobwebs, improved my shaky motor skills, and helped me speak like a fluent person again.
At times, I found the therapy silly. I recall one session in which I was asked to do math using a calculator: How much did a set of grocery items on a shopping list add up to? I punched in the numbers, double-checking that I'd pressed the right button, and then triple-checked the response. I knew that each incorrect answer would be used against me (i.e., as a sign that I was still cognitively deficient), so I did my best to avoid messing up. After doing one set of calculations, the nurse who was with me told me I was wrong. I told her that I knew I was right. She matter-of-factly stated that I was wrong. I asked if I could check my work again. When I did, I got the same answer. I talked out loud so she could hear my thought process. After she took the calculator from me and redid the calculation, she sheepishly said she had made a mistake and that I was right. I wasn't a dummy after all.
Occupational therapy flashcards.
I also found some of the therapy hilarious and surreal. The hospital had a room that was meant to look like a standard apartment. It had a kitchen, a dining table, and all the accoutrements of normal life. My mission, if I chose to accept it, was to cook breakfast, beginning with scrambled eggs, and including toast. I felt awkward putting on a private home economics show, but I did my best to keep my hands steady as I placed the frying pan on the stovetop. Then, I whisked some eggs together and scrambled them. I had proven my worth! (Unfortunately, I had not yet progressed beyond eating a meal predominantly composed of apple sauce, so I didn't have the chance to taste my own creation.)
But mostly, recovery involved sleep. Lots of sleep. Sleep was my default state. All roads led to sleep. If I was bored, I slept. If I was excited, I fell asleep again (probably because I was over-excited). If I was sleepy, I slept. I slept on my stomach. I slept on my back. I slept in my wheelchair. I just kept sleeping.
In the constant cycle of sleeping and waking, I also lost track of time. This was somewhat liberating. But it was also unsettling to think that I had unlatched myself from the regular continuum of life, which proceeds day by day, hour by hour, according to routines and habits and daily rituals--none of which I could maintain while in the hospital.
I benefitted from the constant flow of people. There were my parents, who flew out from Seoul, utterly shocked at the prospect of losing their first son. There was my aunt, herself a doctor, who got another doctor to cover her shifts and her patients, so that I could temporarily become one of hers. There was my girlfriend, who, despite having just undergone surgery herself a couple days earlier, also dropped everything to be by my side. There were my friends--Will included--who made several visits, and some of whom I didn't even know had visited me (because I was still comatose at the time). And then there were all the doctors, and nurses, and nurse practitioners, and all the other people with all the other acronyms and abbreviations and titles and roles and responsibilities and names that I can no longer remember now, even if my life depended on it (but that appear as hidden cast members in my 3-inch stack of medical bills).
I welcomed this flow of people, not least because these were people who mattered to me, and who cared for me, and who cheered me up, but also because it presented a constant flurry of newness that punctuated the dullness of the sterile turquoise greenness that was my hospital room.
In addition to the flow of people, was the flow of flowers, notes, and care packages from friends, family, and coworkers. Somehow, word had gotten around that I was stuck in the hospital, and people from all over the world were sending me things, including a photo album of lots of memorable moments.
My law firm was tremendously accommodating during this time. I was given direct orders by the managing partner to rest up and not spend a single ounce of energy thinking about work. I received many notes from coworkers. I even received an uplifting "get well" video. These little things made a difference.
One thing I didn't benefit from was the hospital food. I would spend tens of minutes perusing the menu, trying to identify foods that sounded appealing, and foods that I knew would sit well in my teetering digestive system. There was often a significant mismatch, and although I aspired to eat the omelette with bacon and croissant, the words that came out of my mouth when I spoke to the food service operator were usually, "I'll take two unsweetened apple sauces, and two bottles of chocolate Ensure. Thanks..."
One of the hardest parts of being cooped up in the hospital was the constant tension between feeling like I was wasting time and feeling like time could not pass any slower. On the one hand, I felt restless and helpless. Being stuck in a hospital bed, practically unable to move, while the whole world passed by was hard to deal with. Even though I knew my body needed rest, I didn't like that I could almost feel my muscles atrophying (in fact, I ended up losing 10 pounds off an already lightweight frame). I was also concerned about my obligations at work. Was I letting my colleagues down by being out of commission for this long? Should I be working while recovering? Was anyone mad that I was gone? The answer to all of these was no, but at times I felt the answer was yes.
At the same time, I also developed the sense that I had way too much time on my hands. I began doing whatever I could to help pass the time. I went onto Amazon Prime and started watching "recommended" movies. Computer algorithms have come a long way, but they weren't good enough here--everything recommended to me was uninteresting. For the first time in a long time, I took control of a TV remote and channel surfed like I had just discovered cable television. I wanted time to speed up, if only so that I could be discharged from the hospital sooner.
After almost a week of being bed-ridden and indoors, the nurse finally let me walk outside. It was still the height of summer, and it was balmy, but I still felt the chills as I waddled through the hospital's doors and into the hospital parking lot. My heart rate shot up with my first steps. I could feel the thump-thump beating in my chest. For the first time in my life, walking was hard. At that moment, the trite saying appeared to be true: "You don't know what you've got until it's gone."
My first walk outside. You can sense my happiness. Also pictured: the helicopter that saved me.
That moment also triggered new anxiety. Would I ever get back what appeared to be gone? Setting aside getting back into peak physical fitness, would I ever be able to run again? No one in the hospital had ever provided a prognosis. In fact, at this point, I barely even knew what had taken me out in the first place. So much had happened while I was still unconscious, and I didn't have any of my medical records at the time. It was disconcerting not knowing whether my current state (of immobility and languor) would be permanent.
In my second week at the hospital, I appeared to take a turn for the better. Suddenly, the pain no longer hovered over me or clouded my thoughts. I had periods where I felt relatively comfortable. I had passed my wheelchair days, and could walk around the hospital practically without assistance. I think I became more chipper at that point. I may have started smiling every now and then. Things were looking up.
Sporting a bigger grin than my brother.
Even the therapy began to go really well. I started to enjoy showing off my calculator skills to the nurse who had essentially called me a dummy earlier. I breezed through the flashcards, crushed the map-drawing exercises, and sorted my pills in the pillboxes like I actually maintained a complicated fifteen-prescription drug regimen. I even got the opportunity to "run" wind sprints (at grandfather pace) down the hallway. I began spending time in the hospital cafeteria, and had the occasional friend pop in for a visit. I was beginning to feel optimistic, and less like the downer I'd been the first week.
Eventually, after 10 days of rest and tests and therapy, I ran through some final procedures--EEGs, x-rays, MRIs--all of which confirmed that I was finally ready to be discharged. I could return home and continue my recovery there, instead of in St. Anthony.
In the process of wrapping things up, I finally got a complete picture on what had occurred on July 10. I'd learned bits and pieces throughout my stay, but this time my doctors walked me through the treatments I'd received and my diagnoses from beginning to end. My jaw dropped after hearing everything.
Among other things, I had developed HACE (high altitude cerebral edema) and HAPE (high altitude pulmonary edema)--two independently deadly altitude illnesses. Altitude illnesses fall along a spectrum. People reaching high altitudes generally experience some form of altitude illness, usually mild or moderate acute mountain sickness (AMS). Symptoms of AMS include dizziness, nausea, headaches. Mostly, AMS is a nuisance. But at the end of the spectrum are HACE and HAPE, and those illnesses are not to be messed with. (This website does a good job explaining AMS, HACE, and HAPE.)
I had first learned about HACE and HAPE after reading Jon Krakauer's classic, Into Thin Air. I always understood HACE and HAPE to fall into the category of the unimaginable, simply because I associated them with extreme mountaineering of the kind described in Krakauer's book. I was not an extreme mountaineer, and couldn't imagine ever having anything to do with HACE or HAPE. I had also never heard of people getting HACE or HAPE at a relatively low 12,000 feet. So I was shocked to learn that I'd somehow developed both conditions.
All of my doctors were shocked too. Apparently, even St. Anthony Hospital--which is the closest major hospital to the Rockies--rarely got patients with HACE or HAPE. Instead, the hospital would frequently receive patients experiencing milder forms of AMS. That is because even the tallest of the Rocky Mountains don't go much beyond 14,000 feet. In other words, in the grand scheme of dangerously tall mountains, the Rockies are relatively safe.
Only when I began flipping through my medical charts and x-rays could I finally see how grim things had been. This x-ray, taken shortly after I arrived in the ICU, shows that my lungs were filled with fluid--my left lung, almost completely--as a result of HAPE:
My first x-ray upon arrival at St. Anthony Hospital.
My x-ray showed nothing close to a normal chest x-ray. I also learned that, in addition to being intubated so that I could maintain an open airway, I had a separate tube inserted into my lungs to suck out the fluid. In my first couple nights, a nearly full bottle of the following substance was pulled out of my lungs:
Fluid sucked out of my lungs.
It was overwhelming to finally learn all the gory details, and to realize just how close to death I had really been. I recall speaking to one nurse who told me that, based on my critical condition when I arrived, the hospital staff was unsure whether I'd make it through that first night. I had been oblivious to this possibility. It was another humbling moment, and another opportunity for me to give thanks to the work of the rescue team and the medical staff.
(Several months after being discharged, my treating neurologist asked for my permission to use my medical records for a case study on high altitude illnesses to be presented to Colorado's top doctors specializing in altitude illnesses. My neurologist told me that both the extreme nature of my condition and the extremely rapid recovery made for a unique learning opportunity. I obviously granted permission. The case study was presented recently. I was able to view the presentation, but am unable to share details about it.)
On the afternoon of July 20, I hobbled out of the hospital with my mom, headed to Denver International Airport, and flew back to D.C. I was finally home.
RECOVERY: D.C.
The second phase of recovery was pretty unremarkable. One of the first things I did while home was test my running legs out. I wanted to set a baseline and help temper expectations on how long it would take to make my running comeback. After what had felt like months, I put on running shoes and headed down to the gym. Given the summer heat and humidity, I opted for a treadmill--something I only use as a last resort. I was determined to run 2 miles at whatever pace felt "safe". I didn't really know what that meant. My doctors had said I could resume normal activity whenever I felt ready. But it was hard to self-assess readiness. Plus, most of the running I did was not in the normal range. In any event, the 2 miles were painful and took over 20 excruciating minutes, a good 2-3 minutes-per-mile slower than my usual "easy" pace. As a runner, I felt like I was back to square one. I tried not to feel discouraged, and told myself to be patient and build back slowly.
Mostly, I spent my first days at home doing more of what I had become good at while at St. Anthony: sleeping. I was too drained to do much of anything else. I spent entire days sitting on my couch, staring at cloud formations out my window. After about a week of drifting in and out of sleep for 15-18 hours per day, I began to feel like I could reincorporate other normal activities into my routine.
I began socializing with people again. I ventured out to get birthday drinks with old colleagues from Baltimore and my November Project DC running family. I met up with a friend visiting from San Francisco. I realized that these social interactions had just as much healing power as sleeping. So, too, did the opportunities to talk through--almost in a therapeutic way--what had happened out in the Maroon Bells only a few weeks earlier.
Catching up over beers at Right Proper Brewing Company.
At the end of July, to help piece together how events unfolded, and also to convey my thanks, I had phone calls with Will, Shane, and Erik to hear their accounts of the night of July 10. I learned that the experience was just as traumatizing for them as it was for me. Separately, I spoke to Mountain Rescue Aspen's director, Jeff Edelson, who had been one of the dozen MRA team members who took part in the mission. Based on his rundown of the rescue, I realized how perfectly everything had happened. I truly could not have asked for a better outcome.
Talking to Will, Shane, Erik, and Jeff made me think about all the what-ifs. I thought about how things could have been different at every step of the rescue process--and specifically how bad things could have been if even one link in the rescue chain had been broken:
- What if I had not noticed that my condition was deteriorating and we'd continued trucking on?
- What if we'd taken option 3 and gotten lost deep in the wilderness?
- What if we hadn't bumped into Erik, Robert, and Shane?
- What if they hadn't agreed to stay with me?
- What if Will hadn't run and driven as fast as he could to get back to Aspen?
- What if Will hadn't called his parents for a second opinion?
- What if Mountain Rescue Aspen had chosen to delay the rescue until daylight?
- What if the helicopter couldn't make a landing?
I also thought about how I might have made different decisions during my trip that might have helped me avoid the incident altogether:
- What if I had flown into Denver and spent a night acclimating there, instead of flying directly into Aspen?
- What if I hadn't gone on that test-run in Snowmass?
- What if we hadn't gone downhill mountain biking that Saturday?
- What if I hadn't had any beers in the lead-up to the run?
- What if we'd been hiking instead of running?
- What if I'd not taken all those ibuprofens when I started getting a headache?
- What if I'd had more water during the day? Less?
- What if I'd recognized my symptoms earlier?
- What if we'd turned around earlier?
It was natural for me to consider all of these hypotheticals. After all, as a lawyer, that’s my job—to consider every path on a decision tree, to visualize every outcome imaginable. It was a humbling thought experiment, but I was glad to go through with it. This mental--and emotional--processing was a crucial part of my recovery.
In early August, I was finally feeling ready to return to normal life. I met with my doctors to get their opinions. My general practitioner was impressed that I'd recovered so well--and so quickly. My neurologist looked over a recent MRI and was surprised by the results. I showed no trace of anything. I was given the green light to return to work, running, and everything else; I was also told that the whole incident did not limit what I could do in the future. Those were encouraging words.
NORMALCY
In mid-August, I returned to work, the truest sign that life had returned to normal. It felt strange being back. I felt like I'd started over at a new job. I told my story, over and over again, to coworkers, friends, family, and strangers.
Normalcy meant building back my routines: run-commuting to work in the morning, lawyering all day, catching up with friends and girlfriend in the evening, and generally just making the most of life when I could.
To my delight, my return to running was better and faster than expected. By the end of August, I was back to running 20-milers in Rock Creek Park on weekends. By October, I was up to running 30-milers, racing a 50K trail race, and even pacing a friend to a fast finish at the Marine Corps Marathon. On December 17--less than 5 months after being discharged from the hospital--I ran my first 100-miler at the inaugural Devil Dog Ultras.
Showing off my belt buckle after finishing my first 100-mile race.
During this return to normalcy, I developed one new routine. At the end of each day, without fail, I thought one thought: I am incredibly fucking lucky.
TODAY + TOMORROW
This routine continues today. Every day, I reflect on how incredible it is to be alive. Today, it is hard even believing that I was on the brink of death exactly one year ago.
People ask me if the the incident changed my outlook on life. The answer is yes and no. I have no plans to quit my career as a lawyer and become a traveling yogi, nor have I all of a sudden become religious. But I now begin each day with more hope and optimism--and end each day with more gratefulness--than ever before. I think those are significant changes.
People also ask me if I'll ever go back into the mountains. The answer is an unequivocal yes. As much as the past year has made me reflect on the value of life, I also know that a well-lived life requires a series of well-calculated risks. The mountains that nearly killed me are also the mountains that have brought so much joy in my life. That's not something I'm willing to give up.
It sounds reckless, particularly after experiencing so much trauma. But to borrow the words of another ultrarunner, "I’m not sure what level of risk is acceptable for me at this point, but I can say that a life of no risk is unacceptable."
For now, I will continue running at less extreme altitudes. But I know for certain that I will be back in the Maroon Bells one day--better prepared, and better acclimated--to complete the Four Pass Loop.